Colposcopy
Mr Chattopadhyay qualified as an accredited colposcopist from The British Society of Colposcopy and Cervical Pathology (BSCCP) in 2012. He has been performing colposcopy for past 5 years.
What is colposcopy?
A colposcopy is a simple procedure used to look at the cervix, the lower part of the womb at the top of the vagina. It’s often done if cervical screening finds abnormal cells in your cervix. These cells aren’t harmful and often go away on their own, but sometimes there’s a risk they could eventually turn into cervical cancer if not treated. A colposcopy can confirm whether cells in your cervix are abnormal and determine whether you need treatment to remove them.
When is a colposcopy needed?
You may be referred for a colposcopy within a few weeks of cervical screening when:
- some of the cells in your screening sample are abnormal
- the nurse or doctor who carried out the screening test thought your cervix didn’t look as healthy as it should
- it wasn’t possible to give you a clear result after several screening tests
- small punch biopsy from the vaginal or the cervical surface
- treatment to remove abnormal cells from the cervix
- removal of cervical polyp
- ablation of vaginal precancerous changes (requires general anaesthetic)
A colposcopy can also be used to find out the cause of problems such as unusual vaginal bleeding (for example, bleeding after sex).
Try not to worry if you’ve been referred for a colposcopy. It’s very unlikely you have cancer and any abnormal cells won’t get worse while you’re waiting for your appointment.
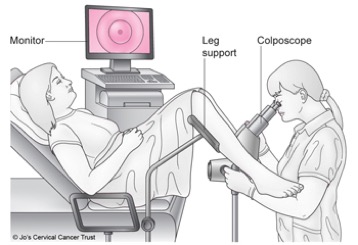
What happens during a colposcopy?
A colposcopy is usually carried out in a hospital clinic. It takes about 15-20 minutes and you can go home the same day.
During the procedure:
- you undress from the waist down (a loose skirt may not need to be removed) and lie down in a special type of chair with padded supports for your legs
- a device called a speculum is inserted into your vagina and gently opened
- a microscope with a light is used to look at your cervix – this doesn’t touch or enter your body
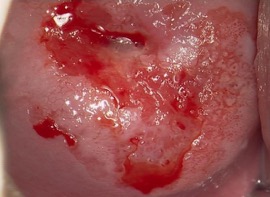
- special liquids (acetic acid and/or Lugol’s iodine) are applied to your cervix to highlight any abnormal areas
- a small sample of tissue (a biopsy) may be removed for closer examination in a laboratory – this may be a bit uncomfortable
If it’s obvious that you have abnormal cells in your cervix, you may have treatment to remove the cells immediately. If this isn’t clear, you’ll need to wait until you get your biopsy results.
What may be the results of a colposcopy?
It’s often possible to tell you right away if there are any abnormal cells in your cervix. But if you had a biopsy, it may take up to four to eight weeks to get your results in the post.
The result of your colposcopy and/or biopsy will be either:
- normal– about 4 out of 10 women have no abnormal cells and are advised to continue attending cervical screening as usual
- abnormal – about 6 out of 10 women have abnormal cells in their cervix and may need treatment to remove them
Mr Chattopadhyay may use the term CIN (cervical intra-epithelial neoplasia) or CGIN (cervical glandular intra-epithelial neoplasia) when discussing your biopsy result. This is the medical name for abnormal cells. It’s followed by a number (for example, CIN 1) that indicates the chances of the cells becoming cancerous. A higher number means a higher risk of cancer developing if the cells aren’t removed.
Treatments to remove abnormal cells
Treatment to remove abnormal cells is recommended if there’s a moderate or high chance of the cells becoming cancerous if left untreated. There are several simple and effective treatments that can be used to remove the abnormal cells, including:
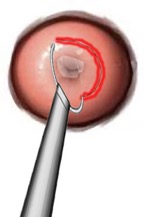
- large loop excision of the transformation zone (LLETZ) – a heated wire loop is used to remove the abnormal cells.
- a cone biopsy – a cone-shaped piece of tissue containing the abnormal cells is cut out from your cervix
LLETZ is usually carried out while you’re awake A local anaesthetic injection is used to infiltrate the cervix before doing this procedure. You can go home the same day. A cone biopsy is usually done under general anaesthetic (where you’re asleep) and you may need to stay in hospital overnight.
What are the risks and complications?
Colposcopy is a very commonly performed procedure and complications are very rare. Minor complications include infection and vaginal discharge and minor bleeding. Serious complications are rare and include heavy bleeding during or after loop biopsy.
After a loop biopsy you will be advised to avoid swimming, baths and penetrative sexual intercourse for 4-6 weeks and also avoid the use of any tampons for a similar duration. The reason for this is to prevent any infection of the raw surface that has just been cauterised. In the event of infection taking place, there is a risk of very heavy torrential bleeding. This requires urgent medical attention. It is normal to have some mild irregular bleeding or discharge after this procedure and this can last anything from 2 to 6 weeks. It is also normal to experience mild crampy discomfort for about 24 to 48 hours which resolves with paracetamol.
What are the long term effects of a loop biopsy?
This biopsy does not cause infertility or difficulty in getting pregnant. However, large studies have shown a minimal increase in the risk of miscarriage especially if more than one loop biopsy has been carried out in your lifetime. As stated, this increased risk is minimal. The vast majority of women who have had this loop biopsy go on to have normal pregnancies.