What is hysteroscopy?
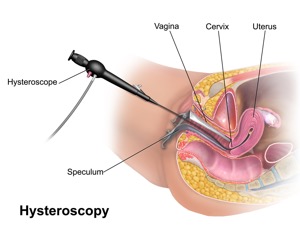
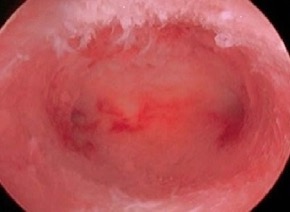
A hysteroscopy is a procedure used to examine the inside of the womb (uterus). It’s carried out using a hysteroscope, which is a narrow telescope with a light and camera at the end. Images are sent to a monitor so your doctor or specialist nurse can see inside your womb. The hysteroscope is passed into your womb through your vagina and cervix (entrance to the womb), which means no cuts need to be made in your skin.
When is a hysteroscopy carried out?
A hysteroscopy can be used to:
- investigate symptoms or problems such as heavy periods, unusual vaginal bleeding, postmenopausal bleeding, by taking biopsy from the cervical canal or endometrium (lining of the womb) –
- diagnose conditions – such as fibroids and polyps (non-cancerous growths in the womb)
- Insertion of MIRENA (http://www.britishfibroidtrust.org.uk/mirena.php)
- treat conditions and problems – such as removing fibroids, polyps, displaced intrauterine devices (IUDs) and intrauterine adhesions (scar tissue that causes absent periods and reduced fertility)
- Endometrial ablation
A procedure called dilatation and curettage (D&C) used to be commonly used to examine the womb and remove abnormal growths, but nowadays hysteroscopies are carried out instead.
What happens during a hysteroscopy?
A hysteroscopy is usually carried out on an outpatient or day-case basis. This means you don’t have to stay in hospital overnight. It may not be necessary to use anaesthetic for the procedure, although local anaesthetic (where medication is used to numb your cervix) is sometimes used.
General anaesthetic may be used if you’re having treatment during the procedure or you would prefer to be asleep while it’s carried out.
During a hysteroscopy:
- you lie on a couch with your legs held in supports and a sheet is used to cover your lower half
- an instrument called a speculum may be inserted into your vagina to hold it open (the same instrument used for a cervical screening test), although this isn’t always necessary
- the hysteroscope is passed into your womb and fluid is gently pumped inside to make it easier for your doctor to see
- the camera sends pictures to a monitor so your doctor can spot and/or treat any abnormalities
A hysteroscopy can take up to 30 minutes in total, although it may only last around 5-10 minutes if it’s just being done to diagnose a condition or investigate symptoms. You may experience some discomfort similar to period cramps while it’s carried out, but it shouldn’t be painful.
How is the recovery following a hysteroscopy procedure?
Most women feel able to return to their normal activities the following day, although some women return to work the same day. You may wish to have a few days off to rest if general anaesthetic was used.
While you’re recovering:
- you can eat and drink as normal straight away
- you may experience cramping that’s similar to period pain and some spotting or bleeding for a few days – this is normal and nothing to worry about unless it’s heavy
- you should avoid having sex for a week, or until any bleeding has stopped, to reduce the risk of infection (see below)
Mr Chattopadhyay will discuss the findings of the procedure with you before you leave hospital.
What are the risks of a hysteroscopy?
A hysteroscopy is generally very safe, but like any procedure there is a small risk of complications. The risk is higher for women who have treatment during a hysteroscopy.
Some of the main risks associated with a hysteroscopy are:
- accidental damage to the womb – this is uncommon, but may require treatment with antibiotics in hospital or, in rare cases, another operation to repair it
- accidental damage to the cervix – this is rare and can usually be easily repaired
- excessive bleeding during or after surgery – this can occur if you had treatment under general anaesthetic and can be treated with medication or another procedure; very rarely it may be necessary to remove the womb (hysterectomy)
- infection of the womb – this can cause smelly vaginal discharge, a fever and heavy bleeding; it can usually be treated with a short course of antibiotics from your GP
- feeling faint – this affects 1 in every 200 women who have a hysteroscopy carried out without an anaesthetic or just a local anaesthetic
A hysteroscopy will only be carried out if the benefits are thought to outweigh the risks.
Alternatives to hysteroscopy
Your womb could also be examined by using a:
- pelvic ultrasound – where a small probe is inserted in the vagina and uses sound waves to produce an image of the inside of your womb
- pipelle endometrial biopsy – when a narrow tube is passed through your cervix into your womb, with suction used to remove a sample of your womb’s lining
These alternatives may be performed alongside a hysteroscopy, but do not provide as much information and can’t be used to treat problems in the same way as a hysteroscopy.