Lichen Planus (LP) affects around 1-2% of the population and is thought to be an auto-immune disease which can affect the skin, oral or genital area and more. The cause is unknown.
Lichen planus is an inflammatory skin disease which commonly causes an itchy rash of small purplish bumps. Often the arms, legs, back or inside of the mouth are affected; however it can also affect the vulva and vagina. Lichen planus may occasionally involve the nail, hair and scalp or the skin around the anus (back passage). Very rarely, it may involve the oesophagus or tear ducts. It is possible to have the disease in one area without ever having a problem elsewhere.
WHAT CAUSES IT?
The cause of lichen planus is unknown. We know that it is NOT caused by infection, hormonal changes or ageing, and is not because of anything that you did or didn’t do. It results from inflammation in the skin. There may be a problem with our immune system, the system that protects a person from infection. In lichen planus the system may be overactive, making proteins that cause inflammation in the skin, mouth or in the genital area. This is referred to as an autoimmune reaction. Occasionally medicines can start this reaction. Why the lesions develop in some places and not others is not known. Lichen planus is NOT contagious and cannot be passed to a sexual partner.
There is no absolute cure for lichen planus. However, in some cases, lichen planus seems to come and go of its own accord and it is possible that it will disappear completely. There are many treatments used to treat lichen planus and treatment needs to be selected to fit your problem. Different people respond to different things. The medications will control but often will not cure the lichen planus. In some cases, usually oral and genital LP, treatment is a long process and close follow up with you and Mr Chattopadhyay is important.
VULVAL / VAGINAL LP
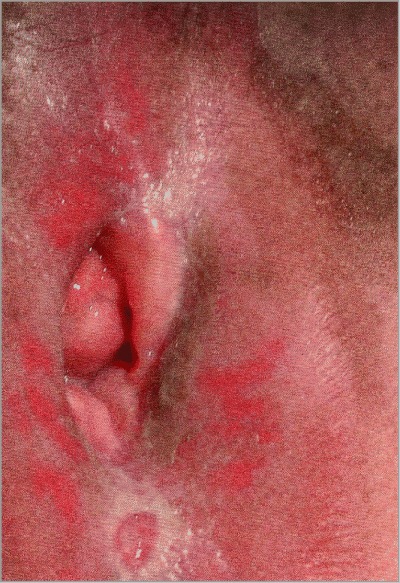
Soreness, burning and rawness are very common symptoms. If the outer layers of the skin break down (erosions), these areas appear moist and red.There may be a white lacy pattern on the vulva.This pattern can also be seen around the edges of the erosions. The vulva may appear pale white or pink/red. Scarring with loss of the inner lips (labia minora) can be seen. The clitoris may be buried under scar tissue.
If the vagina is involved, intercourse can be painful. Erosions can occur inside the vagina in a patchy or generalized pattern. Some women have a sticky, yellow or yellow-green discharge, which can be bloodstained, especially after intercourse. If the two surfaces of the vagina heal together, the vaginal opening can become narrowed. This is one reason why intercourse can be painful. Sometimes it is difficult to perform an internal examination. Rarely, the skin may have thickened areas. These may have a warty appearance.